How to identify and treat red eye
Alexander Thrane

Introduction
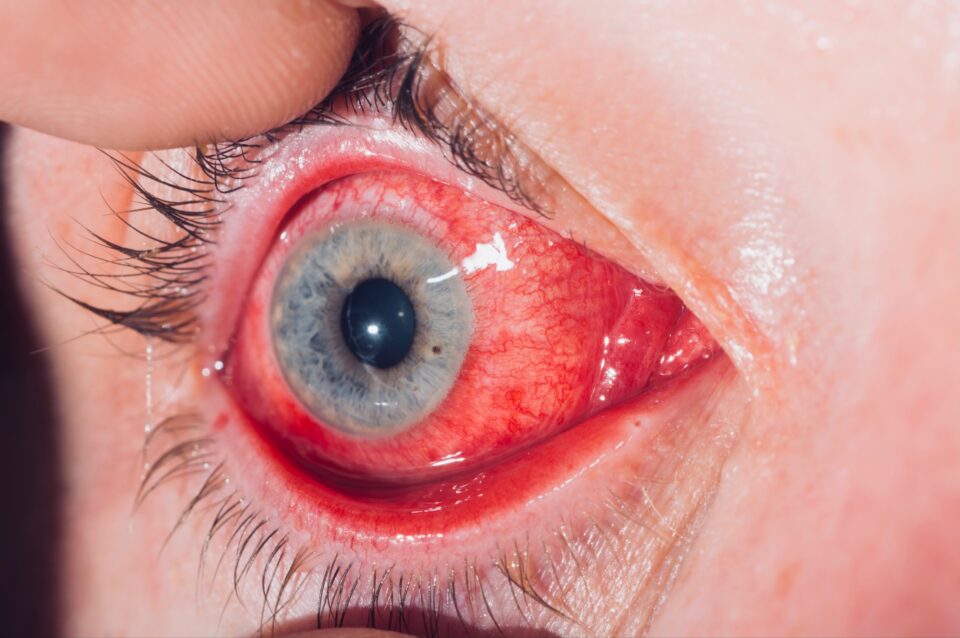
Red eye is one of the most common eye conditions patients report to optometrists. They come in varying degrees of urgency, and in this Expert Conversation, we talk to Dr Alexander Thrane about how to diagnose red eyes, when to refer a patient to an ophthalmologist or GP, and what happens after you’ve referred your patient for treatment.
- Q1 How do the optometrist work structured in the test room when he/she has a patient with red eyes but without symptoms?
- Q2 How do the optometrist work structured in the test room when he/she has a patient with red eyes with symptoms?
- Q3 Can red eyes be an ocular emergency – even if the patient doesn’t have acute pain?
- Q4 Is it possible to distinguish between a virus or a bacteria that causes a red eye, based on clinical observations only and without lab tests?
- Q5 What are the symptoms we need to educate patients on that make a case go from “yellow to red” – so the ones that make it necessary to refer?
- Q6 When should a red eye be referred to a GP and when to the local ophthalmologist?
- Q7 If a case presents with clear symptoms and findings of an allergic conjunctivitis in springtime, is it appropriate to suggest that the patient seeks advice in a pharmacy directly?
- Q8 What should an optometrist do if he/she sees a patient with a red eye a late Friday afternoon and the GP’s and ophthalmologist’s clinics are closed?
- Q9 What is the latest update on red eye being a symptom connected to COVID-19?
- Q10 What does your hygiene routine look like now during the pandemic, when it comes to examining a red eye?
Welcome, Alexander Thrane! Some of our fast Norwegian readers might recognise your name as you gave a lecture in Norwegian on red eyes here on Viewpoint back in November 2020. And today, we’re bringing it to our international readers' attention as well.
So, could you start by telling us how to work structured in the test room when an optometrist has a patient with red eyes but without symptoms?
Yes! When you see a patient, it’s beneficial to use an algorithm to determine the problem, e.g. dividing them based on the following scenarios; red eye with pain, red eye without pain, and other associated symptoms.
They always taught us in medical school that 80 % of the diagnoses rely on good history, and I think the first thing you should do with a patient is just to let them talk and have some open-ended questions ready, to give them 30 sec – 1 minute to explain their problem. Sometimes they come up with things that you would not necessarily think of asking them about.
After that, you go through the essential things. First and foremost, I would rephrase this distinction between with or without symptoms into with or without pain because they might have different causes. An easy way to think after that is to imagine what we call a surgical and anatomical sieve. So basically, try to think systematically about what part of the eye could be affected. That’s an easy way to remember all of the potential causes.
For instance, if it’s a patient without pain, I would also ask about other associated symptoms such as itching or tearing or things like that. Those questions might lead you in one direction; for example, let’s say the patient’s eyes are very itchy, the itchiness is seasonal, and they react to specific allergens. Then you know the cause might be pointing towards allergic conjunctivitis.
And in other cases, you might have patients who have a chronically red eye, but don’t necessarily feel anything because they have reduced sensation. These are more dangerous causes, which means you would have to use the slit lamp to see the exact extent of damage to the eye.
Still, I think that all patients who come in with a red eye would benefit from a pressure measurement. I think it’s mandatory with older patients above 50 years because of the higher prevalence of glaucoma in the elderly population. Also, for younger patients, it could be useful to measure the pressure. Of course, a tonometric measurement might be challenging to achieve, but you can also sometimes just feel it with your fingertips – the normal ocular pressure should feel something like the base of your thumb.
We always need visual acuity to see if the vision is affected in any way or if the refraction is. For instance, if you have an allergic patient with itching, we want to actively search for increasing astigmatism in case he/she has managed to rub himself/herself into getting keratoconus, for example – an associated condition.
And when you look in the slit lamp, I prefer to first look without any eye drops, and that’s no fluorescein initially, because sometimes that can obscure what you’re trying to see, and some changes in the cornea, for instance, can be subtle. And as I also outlined in the lecture, I would try to work from outwards to inwards and think first about the periocular structures – eyelids, lashes etc. Inward facing lashes can, for instance, cause a red eye or an eyelid that’s hanging out or in (ectropion or entropion).
After that, you would work through the tear film and have some opinion about the tear film breakup time and the tear meniscus, and whether you want to do any further tests for this. Then look at the cornea itself. Corneal dystrophies are relatively common, especially basement membrane dystrophies. You can find them in a surprising number of asymptomatic patients if you just look for them. I would then check the anterior chamber to see if any reaction or any cells indicate uveitis. Another sneaky cause of red eye without symptoms in a child who has a swollen joint could be juvenile idiopathic arthritis – it’s a common example of asymptomatic patients but has a potentially dangerous cause of red eye.
Finally, I would look at the lens to see whether there is cataract. Cataract can occur secondary to many of these causes of red eye. In other countries where cataract is allowed to advance further before it’s operated, you can also see a red eye simply from a very advanced cataract that undergoes phacolysis.
You could also look at the fundus to the extent that you feel you can and depending on the tools that you have at hand. So, for instance, if you see a patient with red eye and you suspect the pupil is uneven, and there might be cells in the anterior chamber, and so it turns out it’s uveitis. I have been surprised sometimes that you may also find that uveitis is itself just a symptom of inflammation in the retina, vitreous or the cornea.
And how do the optometrist then work structured in the test room when he/she has a patient with red eyes with symptoms?

So, as we talked about just before, pain is the primary differentiator. And with pain, you want your patients to qualify what type of pain it is because that will help guide you in different directions. Pain that feels like a foreign body on the eye – like sand – usually originated from the cornea, or soreness (dull ache) is more associated with uveitis.
But then there are also patients experiencing extreme pain. And they might as well be misdiagnosed and end up at an entirely different department, like gastroenterology, because they are throwing up from the pain. Such an incident could happen with acute angle-closure – an infrequent but dangerous cause of a red eye with pain and a mid-dilated pupil.
Following up on the last question: can red eyes be an ocular emergency – even if the patient doesn’t have acute pain?

Yes. I gave a couple of examples of this in the lecture too, but just to reiterate, then I would say, if you see a child with a red eye, that would be more unusual because children usually don’t have a red eye without any reason for it.
Especially in the cases where you might expect uveitis, you have to be very careful. Because juvenile idiopathic arthritis – previously termed juvenile rheumatoid arthritis – can cause chronic low-grade inflammation with fewer cells and almost no symptoms. Over time, it can be very damaging to the eye, causing glaucoma, cataract, and potentially blindness in the long term.
Another cause that I also visited was that some patients have a red eye because of a condition that is already damaging their nerves, and therefore they cannot feel the pain. The most common problem would probably be viral infections in the herpes family – so herpes simplex 1 and 2 – and varicella (or CMV) can cause it.
These patients can also develop quite severe corneal scars and potentially perforation because of a neurotrophic cornea – a cornea which you cannot feel when the pain is there, so it’s allowed to dry and get damaged from the environment.
And then there’s also the infrequent cause where some patients are born with an inability or reduced sensation, and they very frequently get severe eye damage from that. But that’s very rare.
Finally, there are patients over 60- or 70-years-old with some slight redness to their eye. Most practitioners probably already know that the most common cause is blepharitis, which is a consequence of ageing, hormonal changes and other things like environmental factors. That’s not very dangerous, but it can be very detrimental to the patient’s quality of life.
Is it possible to distinguish between a virus or a bacteria that causes a red eye, based on clinical observations only and without lab tests?

Yea, I think so. The most exciting thing about the eye – be it within optometry or ophthalmology – is that you can see a lot of detail, and there’s always a lot of interesting things to be discovered.
One of the more common virus infections – so, the chronic recurring virus infections – is the herpes family, which I just mentioned before. They won’t necessarily be associated with a lot of pain. Usually, they will only cause increased tearing without pus, whilst bacterial infection – at least most of the bacteria – tends to cause a very painful ulcer in the cornea and can have quite a significant amount of pus.
Pseudomonas, for instance, is one of the more severe bacterial infections found frequently in contact lens users. The bacteria can generate a lot of greyish pus, which will cause a significant amount of damage to the cornea. Just within a matter of 24 hours, it can deteriorate very quickly.
But with clinical judgement and time, you’ll know what is what. And then I think the other really interesting thing about the question you posed here is how much information we actually get from the laboratory test, right? Because if we take a sample for viral testing and bacterial culture, we usually don’t get the answer until three to seven days later. And by then, you would usually already have had to commence treatment, and once you get the test back, many patients are already in recovery from their problem. Many studies have looked at this particular issue, but the sensitivity and specificity of bacterial culturing aren’t great. Various companies develop multiplex (PCR) platforms that try to give you a more instant answer for the cause, but these are not available in most Scandinavian countries yet.
For instance, patients can be virus-negative (PCR) in the later phases of a herpes virus infection, which can cause a very long course of red eye. And the immunological reaction to the virus is the predominant feature with neurotrophic scars that can cause a deterioration of vision. Sometimes, the patient is PCR-negative at that stage, but it doesn’t mean that they didn’t have a herpes virus infection if everything else fits with the picture.
Not all red eyes are referred, as many mild cases are dealt with by the optometrist. What are the symptoms we need to educate patients on that make a case go from “yellow to red” – so the ones that make it necessary to refer?

Unfortunately, there’s no one solution to this since it depends on the multiple factors that we analyse through our systematic approach to the patient’s history and examination. But some general guidelines would be that if a patient has a severe foreign body sensation, then there is usually an ulcer or epithelial erosion. If that patient is then a contact lens user, the risk of it being a keratitis is so high that I would say this patient group could benefit from an assessment. Especially since keratitis can progress very rapidly on contact lens users – some of the organisms that affect contact lens users can be very aggressive.
And in terms of referral, I think optometrists are in a better position than general practitioners to assess whether it is a keratitis because general practitioners often don’t have a slit lamp. You can learn a lot from a slit lamp and get a lot of information about whether it looks like a bacterial infiltrate or a simple epithelial erosion.
I also think that red eyes that cause a significant amount of photophobia (sensitivity to light), which is usually indicated either by a breach of the corneal epithelium or an intraocular inflammation, can be dangerous and should be assessed by an ophthalmologist.
There are also some less common causes where a red eye should go to an ophthalmologist but they are quite obvious, such as developed proptosis where the eye itself protrudes forward (from the orbit). Then you always have to assess what the cause of the proptosis is.
But I would say with photophobia and severe pain, or foreign body sensation, one should be careful – especially with contact lens users.
When should a red eye be referred to a GP and when to the local ophthalmologist?

In general, I would say that in some healthcare systems, like in the United Kingdom, they do not send eye patients to general practitioners. Instead, they have something called “eye casualty” or just in general more collaboration between optometrists and ophthalmologists. And actually, the UK has a much smaller number of ophthalmologists per capita than all the Nordic countries. I think this system works because general practitioners lack the basic tools to see the details of what’s happening with the eye. Without a (slit lamp) microscope, you cannot see very much with a simple direct ophthalmoscope. The eye patients also represent a small proportion of the patients that a general practitioner sees, so when asked what patients they’ve like to inspect the least, the general practitioners generally say eye patients.
So, I personally don’t think that general practitioners should have such a role in eye care. And in, for instance, Norway, optometrists can refer directly to ophthalmologists. So, I would, at least in the future, hope that a closer collaboration between these two parties would lead to an improvement in eye care.
The only areas where general practitioners could assist in having a larger role would be when the optometrist detects an eye care condition that has implications for the patient’s general health. For example, when the optometrist has taken a photo of the retina and seen that there are signs of high blood pressure or an allergy and on top of that x-number of other things that need systemic medication.
If a case presents with clear symptoms and findings of an allergic conjunctivitis in springtime, is it appropriate to suggest that the patient seeks advice in a pharmacy directly?

Statistically, the most common cause of a red eye is conjunctivitis. The causes of conjunctivitis are primarily bacterial, viral, and allergic, so these are some of the most common things that an optometrist would see. I’m sure most people in practice would agree.
The only issue with medicating and following a person with allergic conjunctivitis is that sometimes allergic conjunctivitis can lead to long-term changes or damages to the cornea. It’s particularly ethnic groups that tend towards specific types of allergic conjunctivitis; giant papillary conjunctivitis or vernal conjunctivitis can cause actual scaring. So, if one is unsure, I think it might be wise for the patient to be assessed by an ophthalmologist.
And then, at least in Norway, patients can receive some of their eye drops on a sponsored or subsidised prescription. The general practitioner can prescribe these eye drops, but they’re usually not as proficient in deciding the correct drop because it’s been a while since they were in medical school.
But I think it all depends on the extent of the problem. If it’s a one-time thing and the patient just wants something that solves the problem – fine. But if the problem recurs or becomes more severe, then I think optometrists should be careful to advise the patient and instead encourage the patient to visit an ophthalmologist.
What should an optometrist do if he/she sees a patient with a red eye a late Friday afternoon and the GP’s and ophthalmologist’s clinics are closed?

Uh, I think it depends on the cause of the red eye. And since the most common cause of a red eye is conjunctivitis – and some of these might need antibacterial eyedrop which cannot be prescribed without a doctor – it’s a bit difficult to treat these patients if they want treatment.
I don’t think this is an issue in, for example, Norway, because if the patient’s own family practitioner is close, then there’s usually an on-call GP department that’s open. Besides that, you can visit an ophthalmologist at the university hospital, which is almost always open.
Still, there are causes of red eye that could easily wait until Monday, such as a very common one like subconjunctival haemorrhage, which is a bleed under the conjunctiva – the eye’s mucous membrane. That usually doesn’t have any dangerous implications. Especially not if there’s not been any significant trauma involved. They can, however, develop spontaneously, particularly with patients that have blood thinners.
Early in the pandemic, there were several articles about red eye being a symptom connected to COVID-19. What is the latest update on this?

Yes, there is a relatively recent systematic review in BMJ (British Medical Journal) where they have collected (and analysed) several papers. I believe it came out in September 2020, so that’s relatively new. There were individual papers that had published slightly diverging or different rates of corona-positivity in conjunctival swabs before that. But the systematic review at least gave us some numbers because it included several other studies, and it seems that about 1 out of 20 patients who are corona-positive have ocular symptoms. The most common cause is conjunctivitis – a viral conjunctivitis like we see with other respiratory viruses. And of those patients, only 1 in 3 had a positive PCR (polymerase chain reaction) swab from the conjunctiva.
One of the reasons why the worry regarding the potential spread of corona via tears has somewhat decreased is that if you multiply these numbers: 1/20 times 1/3, you get 1/60. This means that roughly 1,6 % of patients who are corona-positive would transmit via tears. So that’s a relatively low rate – and actually that’s probably an overestimate as well because the fact that they need to have a positive PCR-reaction from tears doesn’t mean that there needs to be a lot of virus. We need to remember that these tests don’t quantify the amount of virus. So I think the realisation has come slowly but surely that COVID-19 is primarily an airway virus spread by aerosols and not to such a large extent by secretions.
The primary precaution one should take to protect oneself in the clinic is to wear a mask, have a shield on a slit lamp, and try and keep a distance when one is not examining the patient in the slit lamp. And make sure the patient wears a mask too.
It’s also important to have a solid routine for cleaning the slit lamp and all other equipment that comes in contact with the patient every day – for example, by using LiveClean or Virkon or similar agents that denature viruses. But that would be the general recommendation, and I think that’s how the fear has somewhat subsided among our people interested in the eyes.
What does your hygiene routine look like now during the pandemic, when it comes to examining a red eye?

Again, some of the things I mentioned before where everyone wears a mask, and then at Volvat – the private healthcare company that I work within – there’s a mandate that all the doctors and health personnel wear a face shield.
All the equipment that comes in contact with the patient, such as the slit lamp and the examination chairs, need to get a thorough clean every morning, evening and between each patient. That also means we have more extensive use of one-time-use equipment, where previously one might have used more bottled anaesthetic drops and those things.
And then I think rather than having certain routines for red eye patients, you will be better off having these for all patients since there’s such a large number of corona-positive patients that are asymptomatic for airway symptoms rather than from tears. So I don’t think that the red eye would be the best distinguishing factor for when patients have COVID-19. Other symptoms are better distinguishers.
And then there are also other causes of red eye that can be very transmissible and cause small outbreaks, such as adenovirus. So, we try to actively screen patients a little bit when they come in to see whether they might have a viral conjunctivitis of some sort. If they do, then they are taken to a separate examination unit which is primarily for that and gets cleaned. I think this is similar to how they do it in the hospitals.