How to improve your binocular vision testing skills
Betül Tekeli

Introduction
Working as an optometrist and orthoptist in the Netherlands, Betül Tekeli is specialised in the field of binocular vision. That’s why we talk to her about how optometrists and opticians can improve their binocular vision testing skills in this Expert Conversation. What are the essentials you should know about a binocular examination? And when should you refer a patient to an orthoptist or ophthalmologist?
- Q1 What makes binocular vision so interesting for you?
- Q2 When performing a binocular examination, which tests are essential and what are things to look out for?
- Q3 How do the pupil reflexes and accommodation reflexes work?
- Q4 How do amblyopia and strabismus occur, what can be done about it and what’s important to do when you see this in practice?
- Q5 Which patients should you refer a prism?
- Q6 Why and when do you need to refer a patient for cycloplegic refraction?
- Q7 Which advice should you give to children with myopia and their parents, and when do you refer them to an orthoptist?
- Q8 When doing a binocular examination, what are the alarm symptoms to refer a patient immediately to an ophthalmologist?
- Q9 What made you choose for a career in optometry?
- Q10 In your view, what’s the most exciting thing happening in optometry right now? And why?
- Q11 Which books, websites or people inspire you these days?
Thanks for your time, Betül! At Clinical Conference 2020, you hosted a round-table discussion on binocular vision testing and how optometrists can improve their testing skills. So, let’s start at the beginning. What makes binocular vision so interesting for you?

As an orthoptist, you get to see complicated cases – and I like to solve those. Examples are measuring prisms, children with eye problems and cases with more than one binocular problem. Also, I like to work with children, and you get to see many of them with binocular vision problems. The variety of younger and older patients makes the work challenging and fun as well.
When performing a binocular examination, which tests are essential and what are things to look out for?

To start with, asking the right questions to the patient is essential – but that’s of course not just when doing a binocular examination. Ask if the patient has any asthenopic symptoms, like pain around the eyes, headaches, reading problems, dry or watery eyes, blurred vision or vertigo, and if he or she had earlier orthoptic treatment or diagnosis. In the examination, optometrists should check for any manifest or latent strabismus, eye movements, pupillary reflexes, and accommodative problems.
Asking the right questions to the patient or patient is essential – but that’s of course not just when doing a binocular examination.
Okay, let’s dive into the details. How do the pupil reflexes and accommodation reflexes work?

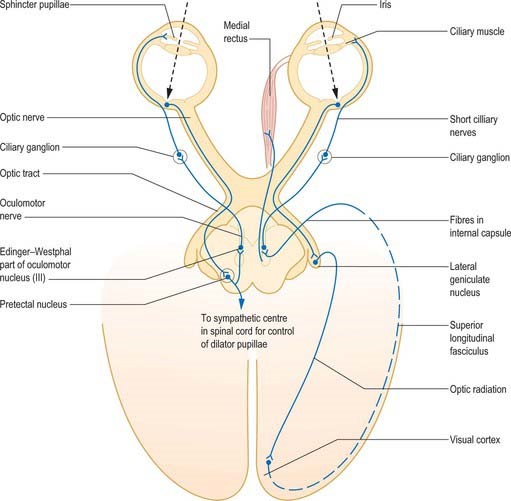
The pupillary light reflex allows the eye to adjust the amount of light reaching the retina and protects the photoreceptors from bright lights. When light falls on the retina, the ganglion cells send a signal to the Edinger-Westphal nucleus in the midbrain. Stimulation of the Edinger-Westphal nucleus causes the stimulation of the sphincter pupillae, which causes pupillary constriction.
Testing the pupillary reflexes is necessary because a few pupillary disorders can lead to problems with accommodation. That’s why you should know if the accommodative problem is not related to a defect in the pupillary reflexes.
The accommodation reflexes, an automatic coordinated change that occurs in the eyes when you switch focus from an object that’s far away to a closer one, are a little bit more complicated. With accommodation, you see that the pupils get smaller, there is convergence, and the lens becomes convex. The pupillary constriction works the same way as with the pupil reflex. The convergence happens because of the musculus rectus medialis that gets stimulated by the third nerve. The stimulation of the musculus ciliare causes the lens to become more convex.
Can you tell a bit more about amblyopia and strabismus? How do these conditions occur, what can be done about it and what’s important to do when you see this in practice?

Amblyopia can have different causes. It can be caused by refractive errors, strabismus, a combination of both, idiopathic and deprivation. It can only be diagnosed if everything else is checked – including the health condition of the eyes. If there’s a difference of two or more lines between both eyes, without any pathology and with the right glasses, we can conclude it’s amblyopia. We know we can treat it best until 8 to 10 years old. First, it’s essential that the child gets the right glasses and patches the good eye to stimulate the amblyopic eye.

Strabismus can be a cause of amblyopia. It can be hereditary, caused by refractive errors, paralysis of the eye muscles, (infectious) diseases, trauma, or cerebral pathology. If there’s also amblyopia, it’s crucial to treat that as well. Also, the right prescription is needed for these patients. If there’s double vision, this can be solved by prisms most of the time. Sometimes, it is necessary to perform eye muscle surgery, especially in young children, to establish binocular vision.

Talking about prisms: which patients should you refer a prism?

For patients with complaints of double vision, prisms can be the answer. However, it is sometimes challenging to prescribe the right prisms. That’s why I think it’s important to refer the patient to an orthoptist if you have any doubts, as a wrong prescription can sometimes do more harm than good.
A wrong prescription can sometimes do more harm than good.
And, why and when do you need to refer a patient for cycloplegic refraction?

There are several reasons why you should refer someone to an optometrist or orthoptist for cycloplegic refraction. To begin with: children between the age of 8 and 10 years old* who’ll get their eyes tested for the first time, because it’s more difficult to measure the eyes of younger children, and because of accommodation it’s important to measure them with cycloplegic refraction. Also, when a patient has reduced vision with unclear or varying refractive errors, or with pre-presbyopes who also have varying or difficult refraction. Other reasons for referral are when younger people have reading problems, or when a patient has headaches (mainly frontal and headaches that occur at the end of the day), or other asthenopic complaints. The main reason to refer these patients is that a wrong prescription of glasses can explain these complaints.
* Please note that this is recommended in the Netherlands. These guidelines might be different in other countries.
Which advice should you give to children with myopia and their parents, and when do you refer them to an orthoptist?

For children with myopia, I believe it’s essential to reduce the activity that involves prolonged near concentration, such as reading a book and looking at a smartphone or tablet, to a maximum of one hour a day. Other pieces of advice are keeping the object at least 30 centimetres from the eyes, resting the eyes every 20 minutes for two minutes, and going outside for at least two hours a day. When there is a high increase compared to a year before (1 dioptre or more), I’d advise to refer them to an orthoptist for myopic control treatment.
Last but not least: when doing a binocular examination, what are the alarm symptoms to refer a patient immediately to an ophthalmologist?

Any of these things should trigger your alarm bells to ring: nystagmus, acquired eye motility disorder, acquired double vision, myopia higher than usual at the patient’s age, and pupillary disorders (except physiological anisocoria).
Over to you! What made you choose for a career in optometry?

I like to help people and give them advice about their eye health when needed. I feel that you can make a real difference as an optometrist. On the other hand, the eye is a complex organ with varying aspects, which makes my job even more enjoyable.
In your view, what’s the most exciting thing happening in optometry right now? And why?

Especially the work with artificial intelligence (AI) is very exciting and interesting. I believe that AI will be the future of optometry – it’s exciting to see that they are so far with this already.
Which books, websites or people inspire you these days?

The last book I read was Atomic Habits by James Clear – I can definitely recommend it. It helped me with building good habits and breaking bad ones.

